BOOK YOUR REFLUX RESOLUTION CALL HERE
Last night I posted this picture on our Facebook wall asking “Why does this baby’s tongue look like this?”
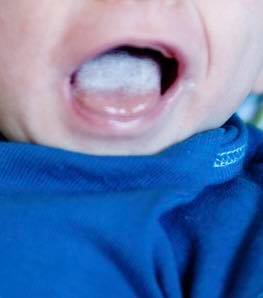
Milky Tongue
I see many similar tongues in clinic, and alongside breastfeeding problems like damaged nipples or pain, they’re typically diagnosed and treated as thrush.
Super resistant, just won’t clear up despite 6 weeks of fluconzole, nystatin and daktarin, hardcore fungus.
Except it’s not.
Well done all the people who guessed this was simply a milky tongue, in a baby who has shallow attachment on the breast or bottle. It doesn’t tell us baby has a tie, or why they’re not attaching effectively, just that they’re not.
When baby attaches effectively and deeply when feeding, the breast fills the mouth entirely sweeping milk and dead skin cells from the area. When they’re not, it doesn’t.
Signs it’s more likely to be a “milky tongue”:
- There is a “stripe” on the tongue and near the tip it’s clean
- The coating can range from a thin even white layer to a thicker coating like the baby pictured.
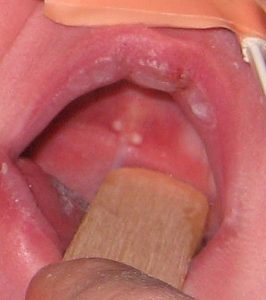
Epstein’s Pearls
- The white areas are limited only to the tongue. Thrush, being fungal is unlikely to be limited to just the tongue as it spreads to other areas such the inside of lips, cheeks and gums. Note, it’s important not to confuse Epstein’s pearls or Bohn’s nodules, which are normal and don’t require treatment.
- Untreated thrush often spreads rapidly
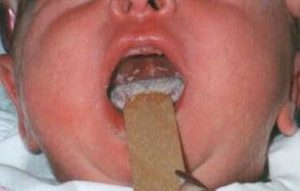
Thrush
- Milk tongue tends to look more white than yellowy (but not always), and in the breastfed baby can also sometimes have a blueish hue (like human milk proteins)
- Gently rubbing small circles with a finger tip, or clean muslin dipped in cooled boiled water may reduce or removes the coating. Note, not all milky tongues are easily wiped away, not being able to do so doesn’t confirm thrush.
Signs it’s more likely to be thrush:
-
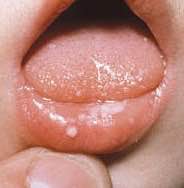
Thrush
Despite the common belief thrush causes a white tongue, in the early stages it can actually be much more subtle. These small isolated spots as seen on the left can be easily missed.
- Thrush can often look in the early stages like little blobs of cottage cheese, progressing to a thick, curdy coating as it establishes (as per the image above).
- Baby may have a whitish sheen to saliva and inside of lips and gums (Mohrbacher & Stock 2003)
- Baby may also have fungal nappy rash
- If left untreated, oral candidiasis will resolve in 3-8 weeks, but in most instances topical antifungal agents are used. Mild cases may be watched without treatment.
Candida is present naturally in many asymptomatic newborns (and adults). An old 1977 paper states that 82% of 140 babies tested were colonised at 4 weeks, thereafter declining slowly to 50% at 1 year. 28 were colonised with the C. albicans (the strain that accounts for about 90% of human yeast infections) at 4 weeks of life and only 3 developed clinical thrush.
If mum has pain it must be thrush right?
Diagnosing thrush in mothers, is more even more complex. Often guidance is to swab mothers, however a 2014 Statement by The National Infant Feeding Network says:
- At least 50% of lactating women will have Staph Aureus on their nipples, many without symptoms (1)
- Staph Aureus and Candida can co-exist
- Standard charcoal skin swabs identified only around 10% of Candida infections in a recent prospective cohort study (1)
- The detection rate in human milk is even lower, due to the presence of lactoferrin in milk (1, 7)
Wendy Jones PhD, MRPharmS and the The Breastfeeding Network (2009) have developed a tool mothers can use to help explore other causes of their pain, and this is an excellent article highlighting the problems that may be mis-diagnosed as thrush.
This information is provided as a guideline. No responsibility can be taken by the author for the way in which the information is used. Clinical decisions remain the responsibility of medical and breastfeeding practitioners. The data presented here is intended to provide some immediate information but cannot replace input from professionals.